Congestive Heart Failure: Insights, Treatments, and the Emerging Role of EECP: Congestive Heart Failure (CHF) is often described as a silent epidemic. It’s a condition where the heart struggles to pump blood efficiently, leading to a cascade of symptoms and complications that can severely affect a person’s quality of life. Despite advancements in medical science, managing CHF remains a challenge, especially as the condition progresses. This blog aims to delve deep into CHF—exploring its causes, symptoms, and treatments—and sheds light on how Enhanced External Counterpulsation (EECP) therapy is emerging as a game-changer in the management of this condition.
What Exactly is Congestive Heart Failure?
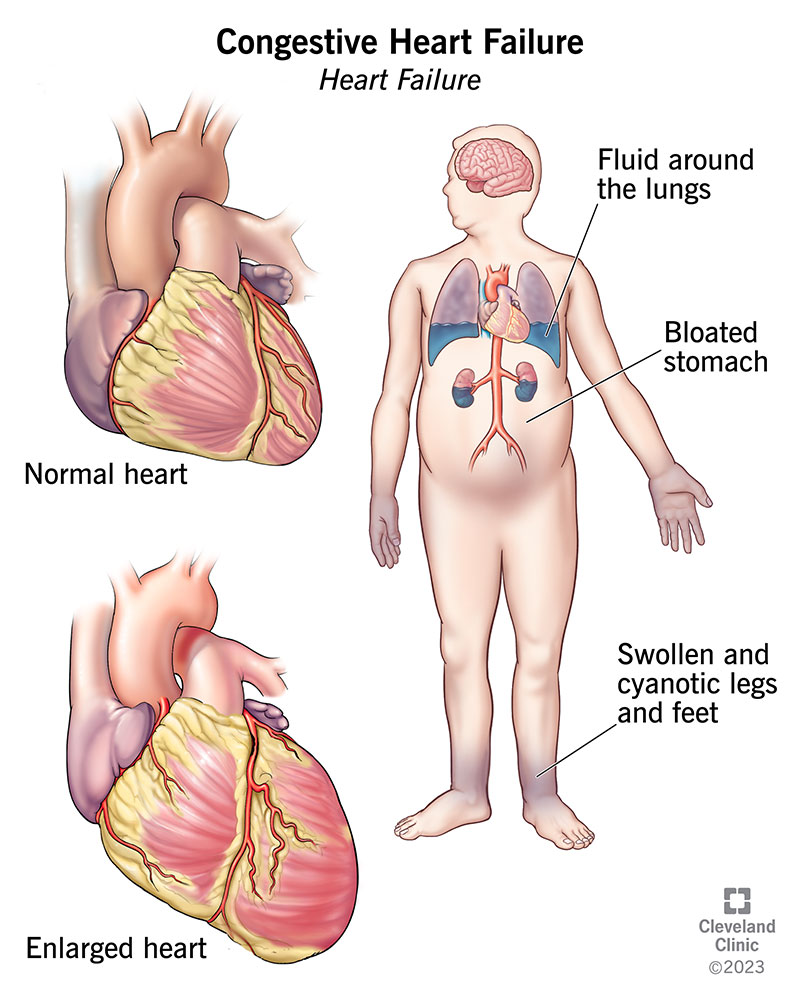
To put it simply, CHF occurs when the heart cannot pump blood effectively. This inefficiency results in blood backing up in other parts of the body, such as the lungs, abdomen, and lower extremities. The term “congestive” refers to the buildup of fluid in these areas, causing symptoms like swelling, breathlessness, and fatigue. CHF is not a disease in itself but a syndrome caused by underlying conditions like coronary artery disease, hypertension, or cardiomyopathy.
How the Heart Loses its Pumping Efficiency
The heart’s job is to maintain a steady circulation of blood. When the heart’s pumping chambers—the left and right ventricles—fail to function properly, it leads to CHF. Depending on the affected side, CHF can be classified as:
- Left-sided Heart Failure: Blood backs up into the lungs, causing respiratory issues.
- Right-sided Heart Failure: Blood backs up into the veins, leading to swelling in the legs and abdomen.
In many cases, CHF affects both sides, making the condition even more complex.
Common Causes of CHF
1. Coronary Artery Disease (CAD)
CAD, caused by plaque buildup in the arteries, restricts blood flow to the heart. This lack of oxygen-rich blood weakens the heart muscle over time, making it a primary cause of CHF.
2. Hypertension (High Blood Pressure)
Consistently high blood pressure forces the heart to work harder. Over time, this added strain causes the heart muscles to weaken or stiffen, reducing their efficiency.
3. Cardiomyopathy
This refers to diseases of the heart muscle, which may result from genetic factors, infections, or alcohol abuse. Cardiomyopathy can significantly impair the heart’s ability to pump blood.
4. Diabetes
Diabetes not only increases the risk of CAD but also contributes to direct damage to the heart muscle, known as diabetic cardiomyopathy.
5. Lifestyle Factors
Sedentary behavior, smoking, obesity, and excessive alcohol consumption are significant contributors to CHF.
Recognizing the Symptoms of CHF
The symptoms of CHF can vary depending on the severity of the condition. However, some common indicators include:
- Persistent shortness of breath, especially during physical activity or while lying down.
- Swelling in the ankles, feet, and abdomen.
- Fatigue and general weakness.
- Rapid or irregular heartbeat.
- Frequent coughing or wheezing, often with blood-tinged phlegm.
- Sudden weight gain due to fluid retention.
If you or someone you know experiences these symptoms, it’s crucial to seek medical attention promptly.
Diagnosing CHF
A combination of clinical evaluation and diagnostic tests is used to confirm CHF. These tests often include:
- Echocardiogram: This ultrasound of the heart evaluates its pumping capacity and measures the ejection fraction (EF).
- Electrocardiogram (ECG): Identifies irregular heart rhythms.
- Chest X-Ray: Detects fluid buildup in the lungs or an enlarged heart.
- Blood Tests: Measure levels of BNP (B-type Natriuretic Peptide), which increase in heart failure.
- Stress Tests: Assess how well the heart performs under physical stress.
Conventional Treatments for CHF
1. Medications
The cornerstone of CHF treatment involves medications, which aim to alleviate symptoms and slow disease progression. Common classes of drugs include:
- Diuretics: Reduce fluid retention.
- ACE Inhibitors/ARBs: Lower blood pressure and improve heart function.
- Beta-Blockers: Decrease heart rate and reduce the heart’s workload.
- Aldosterone Antagonists: Help the body eliminate excess salt and water.
2. Lifestyle Modifications
Adopting a heart-healthy lifestyle is essential in managing CHF. Key recommendations include:
- Following a low-sodium diet.
- Engaging in regular, moderate exercise.
- Avoiding tobacco and limiting alcohol.
- Managing stress and getting adequate sleep.
3. Surgical Interventions
In severe cases, surgical options like coronary bypass surgery, valve repair/replacement, or implantation of a pacemaker may be necessary.
The Role of EECP in Treating CHF
What is EECP?
Enhanced External Counterpulsation (EECP) is a non-invasive therapy that uses external cuffs, placed around the lower limbs, to rhythmically compress the blood vessels. This action improves blood flow back to the heart, reduces the heart’s workload, and enhances oxygen delivery to tissues.
How EECP Works for CHF
- Improves Circulation: By increasing blood flow to the heart, EECP helps reduce symptoms like fatigue and shortness of breath.
- Boosts Collateral Circulation: EECP promotes the development of new blood vessels, providing alternative pathways for blood flow.
- Reduces Afterload: The therapy decreases resistance in blood vessels, making it easier for the heart to pump.
- Enhances Ejection Fraction: Studies have shown that EECP can improve EF in CHF patients, enhancing their overall quality of life.
- Reduces Fluid Congestion: EECP’s effect on venous return can alleviate fluid buildup in the lungs and extremities.
Why Consider EECP?
EECP is particularly beneficial for patients who are not candidates for invasive procedures or who experience limited improvement with medications alone. Its non-invasive nature and minimal side effects make it an attractive option for CHF management.
Success Stories and Clinical Evidence
Numerous studies have highlighted the efficacy of EECP in CHF patients. For instance, research indicates that patients undergoing EECP report significant improvements in exercise tolerance, reduced hospitalizations, and enhanced overall well-being. Real-life success stories further underscore its potential to transform lives.
Addressing FAQs About CHF and EECP
1. Is EECP painful?
No, EECP is a comfortable procedure. Patients may feel the cuffs inflate and deflate, but it is not painful.
2. How long does an EECP session last?
Typically, a session lasts around one hour and is conducted five days a week for seven weeks.
3. Can EECP replace medications?
EECP complements, rather than replaces, standard CHF treatments. It’s vital to continue prescribed medications unless advised otherwise by your doctor.
4. Is EECP covered by insurance?
In many cases, EECP is covered for specific conditions like angina and CHF. Check with your insurance provider for details.
5. Who should avoid EECP?
Patients with severe aortic insufficiency, uncontrolled hypertension, or blood clotting disorders should avoid EECP. A thorough evaluation by a healthcare provider is essential before starting therapy.
Final Thoughts
Congestive Heart Failure is a challenging condition, but advancements in treatments like EECP offer hope for patients seeking better outcomes. By combining conventional therapies with innovative solutions and embracing a heart-healthy lifestyle, individuals with CHF can lead more fulfilling lives. If you or a loved one is living with CHF, consult your healthcare provider to explore the potential of EECP as part of your treatment plan.