Chelation Therapy
Chelation Therapy is an USA – FDA USA-FDA-approved medical Treatment for heavy metal poisoning. Chelation therapy is widely used to treat circulatory disorders, including heart disease, diabetes, and other circulatory disorders.
DETOX Body | Remove Heavy Metals | Improve Circulation
Book your Appointment Now
Book AppointmentNexIn Health - Integrated Health Centre
At NexIn Health, we take pride in being a trusted name in Enhanced External Counterpulsation (EECP) treatment across India. Renowned for our commitment to excellence, NexIn Health is a leading organisation dedicated to providing innovative, non-invasive cardiac care solutions (EECP Therapy in India) and Chelation Therapy in India. Our team comprises highly skilled doctors and healthcare professionals who specialise in delivering cutting-edge heart care through Integrated Therapies EECP therapy, Chelation Therapy, DETOX Therapies, and Other Non – non-invasive treatments, ensuring personalised and effective treatment for every patient.
With a focus on pioneering advancements in non-invasive cardiology, NexIn Health (EECP Treatment and Chelation Therapy in India) is redefining heart care by combining expertise, technology, and compassion. Whether you’re seeking preventive care or advanced treatment, we are here to support your journey toward better heart health. Discover the future of integrated healthcare with NexIn Health – where innovation meets care.
Chelation Therapy in India – Benefits, Risk and Clinical Studies
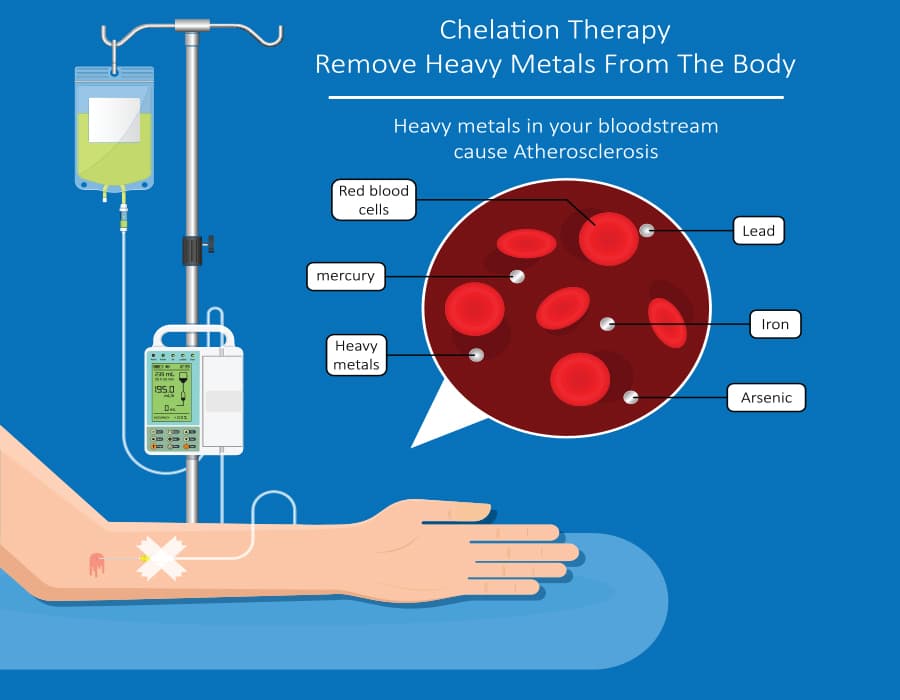
Chelation therapy is an USA – FDA approved treatment for heavy metal poisoning like Lead, Mercury, Arsenic, Mercury, Copper and iron, . Understanding what is chelation therapy and why is it so dangerous or beneficial is crucial for patients considering this medical intervention.
Chelation therapy uses drugs known as chelators to strip toxic metals from within the body and pass them out through urine. This specialized treatment is used for established heavy-metal poisoning and some iron-overload diseases.
Specialists need to oversee its administration because the risk of improper use to cause extensive harm exists. This is particularly important when patients seek chelation therapy in India without proper medical supervision
.
Fact Sheet
- Chelates out poisonous metals such as lead, mercury, arsenic, iron, and copper.
- USA – FDA only approved it for specific heavy-metal poisonings and iron overload when required. Given IV, IM or orally, depending on drug and condition.
- EDTA, DMSA, DMPS and iron chelators are common agents used in professional chelation therapy protocols.
- Potentially lifesaving in acute major poisonings.
- Associated risks are kidney damage, mineral loss, hypocalcemia, and allergic reactions.
- The TACT trial had a modest Cardio Vascular advantage and a larger effect in diabetics. Results are controversial and highlight the benefits of chelation therapy in specific populations.
What is Chelation Therapy in India
Heavy metal toxins can insidiously infiltrate our bodies in the air we breathe, food we consume, or work we perform. Once these metals build up in excess of safe quantities, they can cause damage to essential organs.
Chelation therapy intervenes as a specific cure that removes these toxic metals and defends or restores organ function when toxicity occurs.
Chelation therapy applies specific molecules known as chelators that bind to metals within the body. Having bound, they are dissolved in water and eliminated by the kidneys or through the bile.
Various chelators have an optimal effect on specific metals, and physicians choose the appropriate one for the specific case. Chelation may be administered by IV, injection, or tablet form, depending on the circumstance.
It is an established treatment for heavy-metal poisoning and certain iron overload issues. Since chelators also strip necessary minerals, physicians monitor patients closely and may administer supplements.
Understanding what are the benefits of chelation therapy in india helps patients make informed decisions about this specialized treatment.
https://www.youtube.com/watch?v=Ye8zs2A-6xg&feature=youtu.be
What are Different Chelating Agents:
There are numerous types of chelators, and each is more effective with a given metal and its own safety issues. Following is a brief list of common chelators used in professional chelation therapy practice.
| Chelating Agent | Role / Function |
| EDTA (calcium-disodium EDTA / CaNa2-EDTA) | Used in some of the initial chelation studies; used to treat lead poisoning; used in certain cardiac trials (EDTA-based infusions). |
| Dimercaprol (BAL) | Ancient antidote for arsenic, mercury, and severe lead; evolved for Lewisite exposure. |
| DMSA (Succimer) | Special use for children’s lead poisoning; also for arsenic and mercury in certain environments. Highly recommended by poison centers. |
| DMPS (Dimaval) | For mercury and extreme arsenic in certain nations. |
| Penicillamine | Primary application: copper (Wilson disease); occasionally adjunct for gold, arsenic, lead, rheumatoid arthritis. |
| Deferoxamine / Deferasirox / Deferiprone | Iron-specific chelators for acute iron poisoning and chronic iron overload (e.g., thalassemia). |
| Alpha-lipoic acid (ALA) | A dietary compound with chelating capacity used experimentally; evidence variable. Not a first-line medical chelator according to guidelines. |
Notes: USA – FDA clears only calcium-disodium EDTA and DMSA for lead removal; some agents (DMPS, TTFD) are not FDA cleared.
Chelation takes out some vitamins/minerals from the body while undergoing the treatment, and supplementation is therefore included in the course of therapy.
Patients often ask how much is chelation therapy when considering these different chelating agents.
Health Conditions Treated by Chelation Therapy
As of December 2024, chelation is FDA cleared for only established heavy-metal poisoning and iron overload. Following are the conditions commonly treated with professional chelation therapy:
- Hemochromatosis (excess iron).
- Acute or chronic lead poisoning.
- Mercury poisoning.
- Transfusion-associated iron overload (thalassemia).
- Copper accumulation (Wilson disease).
Why Heavy Metals Accumulate in the Human Body
- Workplace exposure through mining, battery production, or smelting.
- Water contamination from old plumbing (lead) or industrial wastewaters.
- Food contamination (mercury-containing fish, shellfish, rice with arsenic).
- Industrial air contamination.
- Multiple transfusions of blood (leading to iron overload).
- Medications or supplements containing metals.
- Inherited metal-excretion disorders (e.g., Wilson disease).
- Abuse of folk remedies that contain heavy metals.
- Industrial contamination (spills, old paint).
- Release from bone with aging — lead sequestered in bone may be released into circulation.
Understanding these exposure sources helps patients recognize when they might need chelation therapy in India or elsewhere.
Other Possible Usage of Chelation Therapy
Some practitioners recommend chelation for other issues. These are questionable and not commonly recommended. Patients frequently inquire about the benefits of chelation therapy for various conditions:
- Alzheimer’s disease (hypothesis: reduce metal-induced neurotoxicity).
- Autism spectrum disorder (no good evidence; dangerous use reported).
- Diabetes (TACT benefit inferred in diabetics with a history of MI).
- Atherosclerosis / heart disease (previous studies ambivalent; TACT got discussion started).
- Parkinson’s disease (hypothesis-driven; sparse data).
- Hypertension (hypothetical).
- Peripheral artery disease (explored, weak evidence).
- Detox or cleansing (not recommended except in the presence of documented toxicity).
Treatment Administration of Chelation Therapy
Chelation is administered as an IV drip, injection, or tablets, depending on the medication and how rapidly treatment is required.
Clinics operate strictly, beginning with routine tests, gradual infusions, and monitoring vital signs and kidney function.
Most treatment protocols involve mineral supplements and subsequent tests to ensure metals are being eliminated and to prevent deficiencies of essential minerals.
Never take chelation products that have not been prescribed by a doctor. Treatment is only administered when tests indicate high levels of metals, obvious symptoms, and a high probability of benefit.
Patients often wonder how much does it cost for chelation therapy before beginning this intensive monitoring process.
Physicians examine kidney and liver function since chelation is metabolized through these organs. They also review other medications, allergies, heart function, and diet.
For iron excess, specialists choose blood removal or chelation depending on the needs of the patient. Pregnant women and individuals who have serious organ issues require special attention.
Mild or untested “detox” instances typically are not eligible. If a special urine test was utilized, physicians are cautious since it tends to make the level of metals appear greater than it actually is.
Consulting a specialist prior to therapy is recommended, especially when considering chelation therapy in India.
Treatment Procedure:
A general treatment begins with laboratory tests to detect heavy metals, the kidney and liver functioning, electrolytes, and blood counts.
For IV chelation, a qualified practitioner inserts an IV and gradually administers the medicine within 1 to 4 hours, depending on the medication.
Staff monitor vital signs and urine for any early signs of trouble. Oral chelators are swallowed with precise timing and dosing instructions.
Nurses conduct additional laboratory tests after the IV and instruct patients to stay hydrated, take supplements, and be aware of symptoms.
Every session is taped, and emergency action is planned in case of allergic reactions or unexpected changes in blood pressure or calcium.
Sessions are typically done weekly or biweekly, depending on the indication and lab work. Costs vary based on the specific chelation therapy protocol used.
Treatment Duration:
Each IV session is 1 to 4 hours long. Oral treatments vary with the drug and target.
Total treatment duration can be brief, several days or weeks for acute poisoning, or significantly longer for chronic issues such as iron overload.
Treatment in these instances may be from 6 to 24 weeks or even years long for ongoing maintenance.
Treatment can be ended once the metal level is safe and symptoms are resolved, as monitored by routine checks.
For iron overload, chelation or other treatments are needed by some individuals for the rest of their lives, depending upon their risk.
Physicians make the decision to continue or discontinue based upon safety monitoring. Patients should understand what are the benefits of chelation therapy throughout this extended process.
Advantages of Chelation Therapy
Chelation therapy is a powerful advantage when used properly. It sweeps out poisonous metals that attack the brain, liver, kidneys, and heart.
In acute poisoning, chelation is life-saving, stopping damage and improving the prospect of complete recovery.
In chronic conditions, such as iron overload from blood transfusions, it protects the heart and liver, enabling a longer, healthier life.
Several studies, including TACT, have even raised the question of whether metal removal might reduce heart risks in some populations.
Finally, the success of professional chelation therapy is contingent on patient selection with care, appropriate medication, and close monitoring.
Potential Adverse Effects
Chelation therapy is not risk-free, its adverse effects varying from mild discomfort to severe complications. Understanding what is chelation therapy and why is it so dangerous requires knowledge of these potential risks.
Mild symptoms such as nausea, headache, dizziness, or pain at the site of injection can be experienced by some individuals. Very mild fluctuations in blood pressure may also occur.
More serious risks involve kidney injury, abnormally low calcium levels, allergic responses, and loss of necessary minerals.
Excessive or sudden application of EDTA has, in isolated instances, resulted in death.
Such risks make medical supervision stringent, frequent laboratory tests, and mineral supplementation absolutely necessary to ensure patient safety.
Patients with kidney, heart, or liver disease require special precautions prior to initiating any chelation therapy protocol.
Clinical Research and Evidence
Evidence exists favoring chelation for iron overload and heavy-metal toxicity.
In cardiovascular disease, the TACT study demonstrated an 18% reduction in heart issues and additional benefit for individuals with diabetes.
TACT prompted further investigation and controversy, yet subsequent trials were inconsistent so caution is advised, experts say, and conduct more studies.
Health officials advise against the use of chelation for non-approved reasons or without medical supervision.
In general, chelation is established for certain poisonings but remains under trial for most other applications.
More better studies are in progress, particularly examining the benefits of chelation therapy in specific patient populations.
Who Should Have Chelation Therapy
Candidates are those with established, clinically significant metal toxicity or select iron-overload disorders.
Examples: a child with blood lead elevation and accompanying symptoms, or a patient with iron overload due to transfusions with rising ferritin and organ risk.
Candidates should have normal renal function and no contraindications. Specialists weigh risks and benefits, think about alternatives, and decide that monitoring can be done.
Individuals who want “general detox” without objective reasons should be discouraged from chelation.
Always seek opinion from toxicologists, hematologists, or seasoned internists before starting therapy. This applies regardless of whether considering chelation therapy in India or elsewhere.
Who Should Not Undergo Chelation Therapy
Chelation is typically not applied or applied carefully in patients with:
- Advanced kidney disease or renal failure (ineffective excretion of the chelator).
- Advanced liver disease (affects metabolism/excretion).
- Low left ventricular ejection fraction (LVEF <30%) due to risk of instability.
- Active fever or sepsis (increased risk during infusions).
- Hypotension or unstable blood pressure.
- Pregnancy (safety data are generally limited for most agents).
- Severe electrolyte disturbances or malnutrition.
- Documented allergy to the chelator.
- No established toxicity children — EDTA and some agents possess special pediatric risk.
- Incompatible medication patients without clearly defined management.
What to Expect After a Session
After an infusion, patients commonly rest briefly and are discharged the same day.
Some nausea, headache, or fatigue are expected temporarily. Fluids must be consumed to help kidneys rid chelated metals.
Follow any supplement routine to restore minerals. Report immediately if significant symptoms persist like palpitations, severe lightheadedness, shortness of breath, or muscle spasms.
Laboratories will be ordered to monitor kidney function, electrolytes, and levels of metals.
Symptoms may take weeks to improve if metal load was the etiology.
Clinics provide written aftercare information and emergency phone numbers. This helps patients understand what are the benefits of chelation therapy they should expect during recovery.
Popular Other Usage of Chelation Therapy
Chelation Therapy for Heart Health
Chelation for heart disease is of interest to people because metals can hurt blood vessels.
The TACT trial demonstrated a little benefit, and an increased benefit to individuals with diabetes who experienced heart attacks. This hints that metal removal could reduce heart danger in certain individuals.
However, TACT’s findings were controversial, and follow-up studies had variable results.
Large heart associations do not endorse chelation for blocked arteries in place of established therapy such as statins or surgery.
In diabetics with a history of heart attack, chelation can be attempted in studies or specialty centers, but it is not a common treatment.
Patients should carefully consider the benefits of chelation therapy versus established cardiac interventions.
Chelation Therapy in India for Diabetes
It appears some studies indicate chelation can assist individuals with diabetes who have had a heart attack. This may be because they carry more toxic metals associated with blood vessel disease.
In TACT, diabetics experienced a significant decline in risk, and hence more interest and research.
Nevertheless, the evidence isn’t strong enough to utilize chelation for diabetes permanently.
Physicians can take it into consideration as part of research or unique situations but not in place of regular diabetes management. This includes blood sugar, blood pressure, and cholesterol control.
Patients considering this approach often inquire about how much is chelation therapy for diabetic applications.
Chelation Therapy for Autism
A few individuals from alternative medicine have proposed chelation for autism, on the basis of misguided notions that metals are responsible for autism.
Understanding what is chelation therapy and why is it so dangerous is particularly important when discussing autism applications.
Chelation is not known to benefit autism, and it is harmful. Severe injury and even fatalities have occurred among children administered chelation for autism.
Autism is a developmental brain disorder, and the best assistance is from behavioral, educational, and supportive therapies, not chelation.
Chelation for autism can be avoided by parents and physicians, with the possible exception of scrupulous research studies.
Chelation Therapy in India for Cancer
There is no scientific evidence that chelation cures or treats cancer.
There is no scientific support for the claims that chelation takes out cancer-causing metals.
Major cancer groups do not endorse the use of chelation for cancer because it is toxic, damages the kidneys, and interferes with actual treatments.
Patients should be adhering to established cancer therapy and consult their cancer physicians before attempting anything else to prevent harmful effects.
Those exploring alternative treatments often ask about the benefits of chelation therapy, but no credible evidence supports its use in cancer treatment.
Chelation Therapy in India for Peripheral Artery Disease
Chelation has been investigated for peripheral artery disease (PAD) since metals could potentially cause damage to blood vessels.
Studies were inconsistent, and previous work tended not to have tight controls.
TACT and subsequent studies attracted more attention, but chelation is not a standard treatment for PAD yet.
Individuals with PAD must continue using standard therapies while researchers continue to research chelation in controlled studies.
Patients with PAD considering chelation therapy in India should discuss this with their vascular specialists.
Does chelation therapy get covered by insurance?
Insurance coverage varies widely. Many insurers approve chelation only when medically necessary (documented heavy-metal poisoning or iron overload) and after prior authorization.
Elective or alternative uses are usually excluded. Always get written pre-authorization, submit lab reports and physician notes.
Confirm co-pays, exclusions and network rules with your insurer before starting.
Patients frequently ask is chelation therapy covered by insurance, and the answer depends on medical necessity and specific insurance policies.
Cost of chelation therapy in India
Per-session chelation infusions typically cost ₹2,000–₹4,000 depending on drug and facility.
A complete package (multiple sessions, monitoring, supplements, tests) usually ranges ₹40,000–₹150,000.
Final pricing depends on number of sessions, chelator choice, hospital grade and investigations.
Patients wondering how much does it cost for chelation therapy should request an itemised estimate and ask about instalment or insurance support.
The cost of chelation therapy in India remains competitive compared to international rates while maintaining quality standards.
Controversies of Chelation Therapies
Chelation therapy is contentious due to aggressive marketing, safety concerns, and conflicting studies for anything other than the removal of harmful metals.
Others have promoted chelation for heart disease, autism, and cancer with little evidence, causing severe harm and warnings from health authorities.
The TACT study reported potential benefits for some, but subsequent studies and expert reviews have cast suspicion.
The issue is exacerbated by unapproved chelation products available over the counter, which can be hazardous.
Clear regulations, truthful information, and diligence in research must resolve these controversies. This includes understanding what is chelation therapy and why is it so dangerous.
History of Chelation Therapy
Chelation began when EDTA was developed during the 1930s.
In World War II, researchers experimented to cure chemical weapon poisoning, and subsequently discovered that EDTA cured lead poisoning.
Doctors in the 1950s recognized chelation could treat blood vessel issues, spurring decades of controversy and research.
New iron chelators and medications opened up medical application, however, but using chelation for unofficial purposes prompted warning from regulators.
The practice now exists in balance between established uses of toxicology and active research. Ongoing studies examine the benefits of chelation therapy in various medical applications.
Expert Opinion from NexIn Health
In NexIn Health, we regard chelation as a treatment only for established heavy-metal poisoning or iron overload.
We emphasize proper diagnosis, selecting the appropriate medicine on evidence, and vigilant monitoring to achieve maximum benefit at minimum risk.
We do not favor chelation for routine detox or as routine therapy for chronic disease with weak evidence.
TACT results are fascinating but not specific enough for widespread application to heart issues. We endorse chelation for heart conditions only in research or specialty clinics.
Patient safety, laboratory testing, and prevention of new metal exposure are our priorities when administering chelation therapy in India and internationally.
Book An Appointment With Us
Experience top-quality healthcare at NexIn Health Clinic. Schedule your appointment with our expert team today for personalized and compassionate medical care. Book now to prioritize your health and well-being!
Get Appointment With Nexin health
Choose Nexin healthy For Heart
Treatments!
- TAVI/TAVR
- Heart Surgery
- ASD/VSD/PDA Device
- Device Closure
- Angina Treatment
- Heart Failure
- Heart Attack
- Chest Pain
- Hypertension
- Heart Diseases
- Heart Holes Surgery
13 Years of Experience
Our clinic has a rich history of delivering quality care, backed by over a decade of expertise in the field.
25,000 Patients Treated
We have a proven track record of successfully treating a diverse range of patients, demonstrating our commitment to effective and personalised care.
Non-Invasive Treatments
We specialise in advanced, non-invasive treatment options that focus on your well-being without the need for surgical procedures.
Frequently Asked Questions (FAQs) for Chelation Therapy in India



