How Dehydration Affects Blood Pressure and Blood Circulation
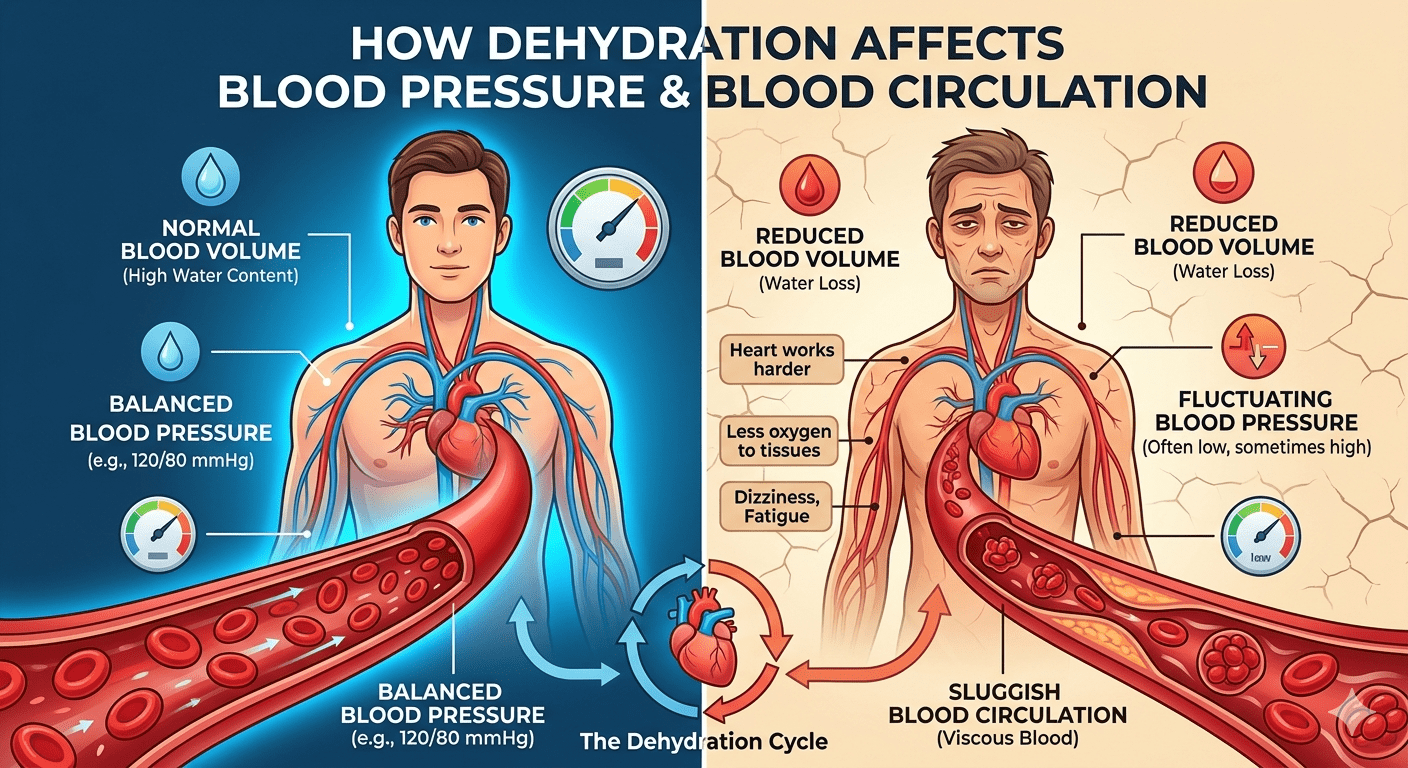

Dehydration and blood pressure are closely linked — yet many heart patients do not realize how dangerous even mild dehydration can be. When your body does not have enough water, your blood volume drops, your heart works harder, and your blood vessels struggle to carry oxygen to every part of your body. For people living with heart disease, diabetes, or metabolic disorders, this combination can trigger serious health problems very quickly.
Whether it is a hot summer afternoon or a busy day when you forgot to drink water, the effects of dehydration on cardiovascular health can be sudden and severe. Understanding how dehydration and blood pressure interact is the first step to protecting your heart.
| ★ Your body is about 60% water — losing even 2% of it can cause measurable drops in blood pressure and mental focus. |
| ★ A Harvard study found that people who drink 5 or more glasses of water daily have a significantly lower risk of fatal coronary heart disease. |
| ★ Dehydration can thicken your blood, making it up to 10% harder for your heart to pump it through your arteries. |
| ★ In summer, sweat can remove over 1 litre of water per hour — putting heart failure patients at high risk within minutes. |
| ★ The kidneys release a hormone called vasopressin during dehydration, which causes blood vessels to tighten — this can spike blood pressure dangerously in heart patients. |
| ★ Mild dehydration is one of the most overlooked triggers for irregular heartbeat (arrhythmia) in older adults. |
Dehydration happens when your body loses more water than it takes in. This can happen due to sweating, vomiting, diarrhoea, not drinking enough fluids, or taking certain medicines like diuretics (water tablets), which are commonly prescribed for heart failure patients.
For people with heart disease or diabetes, dehydration and poor blood circulation are a dangerous combination. The body immediately tries to compensate by narrowing blood vessels and raising heart rate. These responses are helpful short-term, but they put extra stress on an already vulnerable heart.
Dehydration and blood pressure share a direct relationship. Here is what happens inside your body when you are dehydrated:
This is why can dehydration cause high blood pressure is one of the most searched questions — and the answer is YES, it can, especially in people with kidney disease, diabetes, or chronic heart conditions.
Dehydration and low blood pressure symptoms often appear together. Recognising them early can save lives, especially in summer months when fluid loss is rapid.
Important: Heart patients who feel any of these signs should sit down immediately, drink water slowly, and contact their doctor.
Dehydration and poor blood circulation go hand in hand. When the body is low on water, blood becomes thicker and more concentrated. This sticky, thick blood moves slowly through the blood vessels and tends to form clots more easily.
According to recent clinical trials, how dehydration impacts blood flow is most visible in the small blood vessels (capillaries) of the heart, brain, kidneys, and legs. Poor circulation in these areas means that vital organs receive less oxygen and nutrients — which can lead to organ damage over time.
Effects of dehydration on heart health include increased risk of deep vein thrombosis (DVT), peripheral artery disease, and even stroke — all caused by sluggish, thickened blood.
Symptoms of dehydration affecting heart health can sometimes be confused with other cardiac conditions. Knowing the difference is very important:
These are also key signs of dehydration in the body that every heart patient must learn to identify quickly.
Importance of hydration for heart health cannot be overstated, especially for patients who are on medications like ACE inhibitors, beta-blockers, or diuretics. However, heart failure patients must be careful — drinking too much water too quickly can also be dangerous.
Here is a simple daily water intake guide for heart patients:
How water intake affects blood circulation is simple: more water = lower blood viscosity = easier blood flow = less strain on the heart.
Following proper summer care tips for heart failure patients can prevent hospitalisation during hot months. Heat increases sweating, which rapidly depletes body fluids and electrolytes.
Dehydration and cardiovascular health are inseparable. Chronic, repeated episodes of dehydration can silently damage the heart and blood vessels over months and years. Some long-term risks include:
Along with drinking enough water, several natural and traditional remedies can support hydration and heart function:
Note: Always consult a qualified practitioner before starting any herbal, Ayurvedic, or homeopathic treatment, especially if you are on cardiac medications.
Enhanced External Counterpulsation (EECP) Therapy is a cutting-edge, non-invasive treatment for heart patients who suffer from reduced blood circulation, angina, or chronic heart failure. It is particularly useful when dehydration and poor circulation have caused long-term damage to the coronary blood vessels.
During EECP therapy, special cuffs are placed around the legs and buttocks. These cuffs inflate and deflate in sync with the heartbeat, pushing blood back into the coronary arteries and creating new tiny blood vessels (collateral circulation) that bypass blocked ones.
EECP therapy is available at NexIn Health and has helped thousands of heart patients regain their quality of life without invasive procedures.
| Treatment Option | Type | Best For | Risk Level | Availability |
| Oral Rehydration (ORS/Water) | Natural | Mild dehydration | Very Low | Home / Clinic |
| IV Fluid Therapy | Medical | Severe dehydration | Low (in hospital) | Hospital only |
| Anti-hypertensive Medicines | Pharmaceutical | High BP episodes | Moderate (side effects) | Prescription needed |
| Ayurvedic/Herbal Remedies | Natural / Herbal | Mild-Moderate BP issues | Low (with guidance) | Specialist needed |
| EECP Therapy | Non-Invasive Medical | Chronic poor circulation, angina, heart failure | Very Low | NexIn Health & select centres |
| Lifestyle Changes (diet, hydration, exercise) | Preventive | All patients | None | Self-managed with guidance |
Seek emergency medical help right away if you or a heart patient you know experiences:
Que: Can dehydration cause high blood pressure in heart patients?
Ans: Yes. When you are dehydrated, the body releases hormones like vasopressin and angiotensin that tighten blood vessels. This raises blood pressure. For heart patients, this sudden rise can be very dangerous and increase the risk of heart attack.
Que: What are the first signs of dehydration affecting heart health?
Ans: The earliest signs include dry mouth, dark yellow urine, increased heart rate, dizziness, and fatigue. If you notice these symptoms, start sipping water slowly and rest in a cool place.
Que: How much water should a heart failure patient drink per day?
Ans: Most heart failure patients are asked to restrict fluids to 1 to 1.5 litres per day to avoid fluid overload. However, your doctor will give you a specific target based on your condition. Never adjust your intake without medical advice.
Que: Is coconut water safe for heart patients with high blood pressure?
Ans: Coconut water is generally safe and beneficial because it is rich in potassium, which helps lower blood pressure naturally. However, patients on potassium-sparing diuretics or with kidney disease should check with their doctor first.
Que: Can dehydration and poor blood circulation lead to a blood clot?
Ans: Yes. Dehydration thickens the blood, which slows circulation and increases the chance of clot formation. Blood clots in the legs (DVT) or lungs (pulmonary embolism) are serious risks for dehydrated heart patients.
Que: What are the best summer care tips for heart failure patients?
Ans: Drink water regularly before feeling thirsty, avoid outdoor activity during peak heat hours, wear light clothing, use electrolyte drinks like ORS or diluted buttermilk, and monitor daily weight for sudden fluid gain.
Que: Are there any natural ways to maintain blood pressure during dehydration?
Ans: Yes. Drinking water with a pinch of salt and sugar (a simple ORS), consuming foods rich in potassium (bananas, coconut water), and herbs like hibiscus tea can help stabilise blood pressure. Always combine with medical treatment.
Que: How does dehydration and cardiovascular health relate in diabetes patients?
Ans: Diabetes can cause excessive urination (polyuria), which accelerates dehydration. This raises blood glucose concentration further, strains the kidneys, and thickens the blood — creating a dangerous cycle of dehydration, poor circulation, and heart stress.
Que: Is EECP therapy suitable for elderly heart patients with dehydration-related heart disease?
Ans: EECP therapy is a safe and well-tolerated option for elderly patients. It improves blood flow naturally without surgery or medication changes. Your doctor at NexIn Health will assess your complete condition before recommending it.
Que: Can Ayurvedic treatments replace heart medications for blood pressure management?
Ans: No. Ayurvedic and herbal remedies should only be used as a complementary support alongside your prescribed cardiac medications, never as a replacement. Always inform your cardiologist before starting any herbal supplement.
Que: What electrolytes are most important for heart patients to prevent dehydration effects?
Ans: Sodium, potassium, and magnesium are the three most important electrolytes. Imbalance in any of these — especially potassium — can trigger arrhythmia (irregular heartbeat) in heart patients. ORS, coconut water, and doctor-advised electrolyte supplements can help.
| 💙 About NexIn Health — Expert Care for Your Heart and Spine
NexIn Health is a trusted centre specialising in Heart and Spine treatment using Non-Invasive Integrated Techniques. With over 14 years of experience and more than 30,000 patients consulted, NexIn Health offers evidence-based, drug-free solutions including EECP Therapy, to help heart patients live better without surgery. 📞 Phone & WhatsApp: +91 93101 45010 🌐 Website: www.nexinhealth.in 📧 Email: care@nexinhealth.in Book your consultation today — Your heart deserves the best care. |